March 1 - 31, 2026: Issue 652
Latest quarterly report shows NSW public health system experiencing record demand: Data
March 11 2026
The Bureau of Health Information (BHI) has today released its latest Healthcare Quarterly report, showing activity and performance for public health services in NSW from October to December 2025.
NSW public hospital and ambulance services experienced increased demand during the quarter, with record numbers of emergency department (ED) attendances, admitted patient episodes and ambulance calls, incidents and responses.
BHI Chief Executive, Adjunct Professor Heiko Spallek, said: “Despite unprecedented demand across the NSW public health system, performance remained stable in key areas.”
There were 820,009 attendances at NSW hospital EDs during the quarter – the highest since BHI began reporting in 2010. There was an increase in presentations for the more urgent clinical conditions (triage categories 1, 2 and 3), while fewer patients presented with less urgent conditions (triage categories 4 and 5).
The percentage of patients starting their treatment on time (66.3%) was relatively stable compared with the same quarter a year earlier. The median time patients spent in EDs from arrival to leaving was 3 hours and 46 minutes – up 12 minutes. A record number of patients (79,004) left NSW hospital EDs without, or before completing, treatment – up by 10,846 (15.9%) from the same quarter a year earlier.
Ambulance services also experienced record demand, with the highest number of calls and incidents since 2010. While the number of ambulance responses was relatively stable (up 0.6%) compared with the same quarter a year earlier, it was also a record high.
The percentage of ‘life-threatening (CAT 1)’ responses within 10 minutes was 61.6% and the median response time for CAT 1 was 8.5 minutes, both relatively stable.
There were 518,436 admitted patient episodes during the quarter – the highest of any October to December quarter since 2010. While the average length of stay for all overnight episodes was relatively stable (6.2 days), the average length of stay for overnight non-acute episodes (e.g. rehabilitation, geriatric evaluation and management) was 19.3 days – the highest of any October to December quarter.
The number of elective surgeries performed (58,922) was up 7.2%, with more surgeries performed across all urgency categories.
The percentage of elective surgeries performed on time (83.1%) was relatively stable. However, patients who received non-urgent surgery had a median wait time of 324 days, up 15 days from the same quarter a year earlier.
At the end of December 2025, there were 92,812 patients on the waiting list, down 7.4% from the same time a year earlier. Of those patients, 3,845 had waited longer than clinically recommended, down 43.8% from the same time in 2024.
Stranded commonwealth patients surge
The NSW Government stated the improvements in hospital performance has been offset by a surge in the number of stranded patients waiting in our hospitals for Commonwealth aged care or NDIS placements.
The number of stranded patients in NSW public hospitals has increased by 50 per cent over the year to 31 December 2025.
The number of patients ready to be discharged but waiting for a commonwealth aged care placement has almost doubled from 438 to 776.
The number of stranded patients in Western Sydney has almost doubled, with the number of stranded patients at Westmead Hospital more than doubling.
The number of stranded patients in South West Sydney has increased by over 50 per cent, with the number of stranded patients at Liverpool Hospital more than tripling.
The number of stranded patients in the Illawarra South Coast has increased by almost 30 per cent, with the number of stranded patients at Wollongong Hospital doubling.
As at 31 December 2025, bed block was responsible for the loss of 67,680 bed days – up from 41,345 in December 2024 – meaning not only are stranded patients increasing in our hospitals, they’re also waiting longer.
Minister for Health, Ryan Park said:
“Our hospitals continue to show signs of progress and improvement in terms of ED and surgery wait times, which has coincided with our investments in more hospitals, more staff, and more pathways to care outside of the hospital.
“We’re focused on saving our EDs for the patients who need it most while sparing people who don’t require emergency care an unnecessary wait.
“These improvements however are being offset by commonwealth bed block – patients ready to be discharged but unable to leave because they are waiting for Commonwealth aged care or NDIS placements. They deserve better.
“I am so grateful for the additional help and assistance our federal colleagues announced last week, but there is more work to be done.”
On March 6, 2026 the Australian Government announced it is delivering more aged care beds where they are needed most, to ensure every older Australian can access the world-class aged care they deserve.
'Today, the Government is announcing an additional investment of $115 million through the Aged Care Capital Assistance Program (ACCAP) to rapidly increase access to residential aged care in select hotspots.' the government said
Adelaide, Illawarra, Perth and the Hunter are the four areas to be targeted in this additional funding round starting immediately.
An Expression of Interest process is encouraging interested providers to put forward proposals that will build and open more beds within two years to help address immediate delayed discharge pressures on hospitals, and deliver services that align with the National Aged Care Design Principles.
This latest injection will take funding through the ACCAP program to over $1 billion since 2022. Future ACCAP rounds will follow later this year to ensure the Government continues to kickstart projects in regional areas.
The process will be split into two phases, with the first EOI, covering Adelaide and Illawarra, to open on Friday, 13 March and the second to focus on Perth and The Hunter to follow. Interested providers will have six weeks from opening to submit their EOI.
EOI documents, including instructions on how to participate, are available on GrantConnect.
Minister for Health, Disability and Ageing, The Hon. Mark Butler MP said:
“The Albanese Government is making record investments to increase the supply of beds and capacity of our aged care systems to ensure every older Australian gets the dignity of care and support they deserve.
“We know we face a big challenge in increasing bed capacity across our health and aged care systems to meet growing demand, and that is why we’re investing so strongly to increase supply as quickly as possible.
“Our Government has already invested $1 billion in expanding bed capacity in the aged care system and this latest round of funding will increase supply in areas that need it most, like Adelaide.”
Minister for Aged Care and Seniors, Sam Rae MP stated:
“The Albanese Government is on a mission to deliver more beds, faster and in the places they are most needed – so older Australians and their loved ones have confidence that they can be cared for with dignity, when they need it.
“This announcement is the culmination of our methodical work to identify areas where bed capacity is most urgently needed, and we’re moving quickly to fix it.
“We want every older Australian to access the care they need and get it sooner and closer to home. That’s exactly what this round is aimed at doing – improving access as fast as possible.
“We’ve already invested $1 billion in aged care capital through ACCAP – more than any previous government, and we’ll continue to invest in aged care supply as our ageing population grows.”
South Australian Minister for Health and Wellbeing, Chris Picton MP said:
“South Australia welcomes the Albanese Government’s investment in additional Federal aged care capital funding.
“We are pleased that Adelaide will be among the first places in Australia to receive this additional funding, because this is needed to reduce the aged care bed block.
“The Federal Government’s important investment will complement the Malinauskas Government’s $250 million interest-free loans policy for providers to build new aged care centres, and our plan to develop a new 600-bed aged care precinct at the old Women’s and Children’s Hospital.”
AMA (NSW) response to the BHI quarterly report (Oct–Dec 2025)
Statement by AMA NSW President Dr. Kathryn Austin:
''If today’s Bureau of Health Information Healthcare Quarterly report for October to December 2025 was your bank statement, you’d be very happy with the trajectory of the numbers.
Tragically, it is not.
Ambulance call outs and emergency department attendances were the highest we have seen since the BHI began reporting in 2010.
A record number of patients walked out without starting or finishing treatment in an ED during this reporting period – an incredible 79,000 people – a rise of almost 10,000 in a year. This is highly concerning given almost 35 per cent of those were in triage category 3 – needing urgent care for potentially life-threatening conditions and unsuitable to be treated at an urgent care centre.
People needing non-urgent elective surgery waited longer, and we only saw more elective surgeries performed in this quarter than the same quarter last year only due to the assistance of the private health system.
Yet again, we have a system in crisis. And yet again, we are not seeing any tangible plans from the NSW Government to deal with the rising tide of patients needing hospital care for increasing complex issues.
We know that many patients who receive appropriate primary health care can avoid costly hospital admissions. However, we need a clear plan for challenging tackling chronic issues such as obesity and diabetes before they reach our hospital corridors. If governments are serious about easing pressure on hospitals, they must implement the Special Commission of Inquiry into Healthcare Funding Inquiry’s recommendations and invest properly in prevention.
We know our hospitals are under-funded and funded for getting people through faster rather than delivering the high-stakes, complex care so many patients now require but where is the increased budget and workforce development plans beyond employing new doctors and graduate nurses?
We know that while elderly and NDIS patients are languishing in acute care hospitals due to a lack of beds in aged care facilities and disability homes, but they are not singularly responsible for the logjam in our public hospitals. Under-funding, under staffing and lack of vision in preventative care play significant roles – all under the control of the state government – and the NSW Health Minister knows it.
We repeat our urgent call for an end to boom or bust funding; investment in public hospitals; more consultant doctor positions; modernised industrial arrangements to attract and retain doctors; and the funding of preventative health measures.
The system needs help now. Let’s stop playing politics with people’s lives.''
Activity and performance profiles: Northern Beaches Hospital Data - Mona Vale Hospital no longer listed
These profiles provide an overview of selected activity and performance measures for NSW, individual hospitals, local health districts and hospital peer groups. Information is provided for emergency departments, elective surgery and admitted patients. More detailed results are available in the BHI Data Portal.
Compare previous quarter data in January 2026 report: Northern Beaches Hospital to Transition to Northern Sydney Local Health District (NSLHD) on April 29 2026 - Dee Why Medicare Urgent Care Clinic Now open - Bed Block Surges in NSW Hospitals - ED performance improves but more to do: BHI reports
Related March 2 2026 announcement and update: Private Services to stay at Northern Beaches Hospital
Mona Vale Hospital is no longer listed in this public hospital data as there is no emergency department at the MVH campus. While the Northern Sydney Local Health District may point to presentations, no specific data for the Mona Vale Hospital, and who is currently using the facilities, is in the report.
Pittwater residents protested for years against the closure of the ED at MVH
As of mid-2025, Mona Vale Hospital had completed a major reconfiguration, with successive governments establishing a specialist centre for sub-acute, rehabilitation, and community health services on the site.
Key features include a 20-bed Palliative Care and Geriatric Evaluation Management (GEM) unit, and a refurbished Urgent Care Centre.
Operating within the former Emergency Department, the UCC provides non-acute, walk-in care. It was the first in NSW to roll out the Emergency Care Assessment and Treatment (ECAT) protocol in 2025.
BreastScreen Mona Vale
The Chief Executive’s Board Report of October 2025 states the new BreastScreen NSW site at Mona Vale Community Health Centre officially opened on 25 August 2025. Since commencing operations in June, the service has provided breast screening to over 1,400 clients. Notably, nearly 30% of these clients were attending BreastScreen for the first time, highlighting the site's success in reaching previously underserved population.
That same October 2025 report states:
Disability Strategy
The Disability Strategy team continues to drive initiatives to improve healthcare experiences for people with complex disability support needs. A recent review session with key stakeholders supported the proposal to establish an online Disability Provider Forum to influence provider behaviour. Collaboration with the Emergency Department to Community (ED2C) Team is also underway to address service gaps for individuals whose needs exceed typical NDIS-funded supports. Feedback was provided to the Department of Communities and Justice on foundational supports for children aged 0–8 years with developmental delay or autism, informed by input from NSLHD paediatric and allied health services. Efforts are ongoing to enhance data collection through the Electronic Medical Record (eMR) system, aligning with recommendations from the Disability Royal Commission. Additionally, tailored NDIS-related support and training were delivered to staff across multiple sites, including Royal Rehab, Mona Vale Hospital, Macquarie Hospital, and paediatric services, to strengthen care for individuals with complex needs.
Allied Health Research
The Allied Health Research Team continues to support research capability across NSLHD through a range of initiatives. The Allied Health Research Education Series has commenced, with sessions focused on writing and presentation skills to build clinician confidence in research dissemination. One-on-one research support remains in high demand, with nine individual sessions delivered in the past month. Interdisciplinary research brainstorming sessions have been held at Ryde, Hornsby, and Mona Vale hospitals, identifying opportunities aligned with the new NSLHD research strategy. The team is also contributing to broader strategic initiatives, including input into the National Health and Medical Research Strategy. Monthly newsletters continue to highlight emerging clinician researchers and recent achievements across the district.

Mona Vale Hospital in April 2015. Photo: A J Guesdon
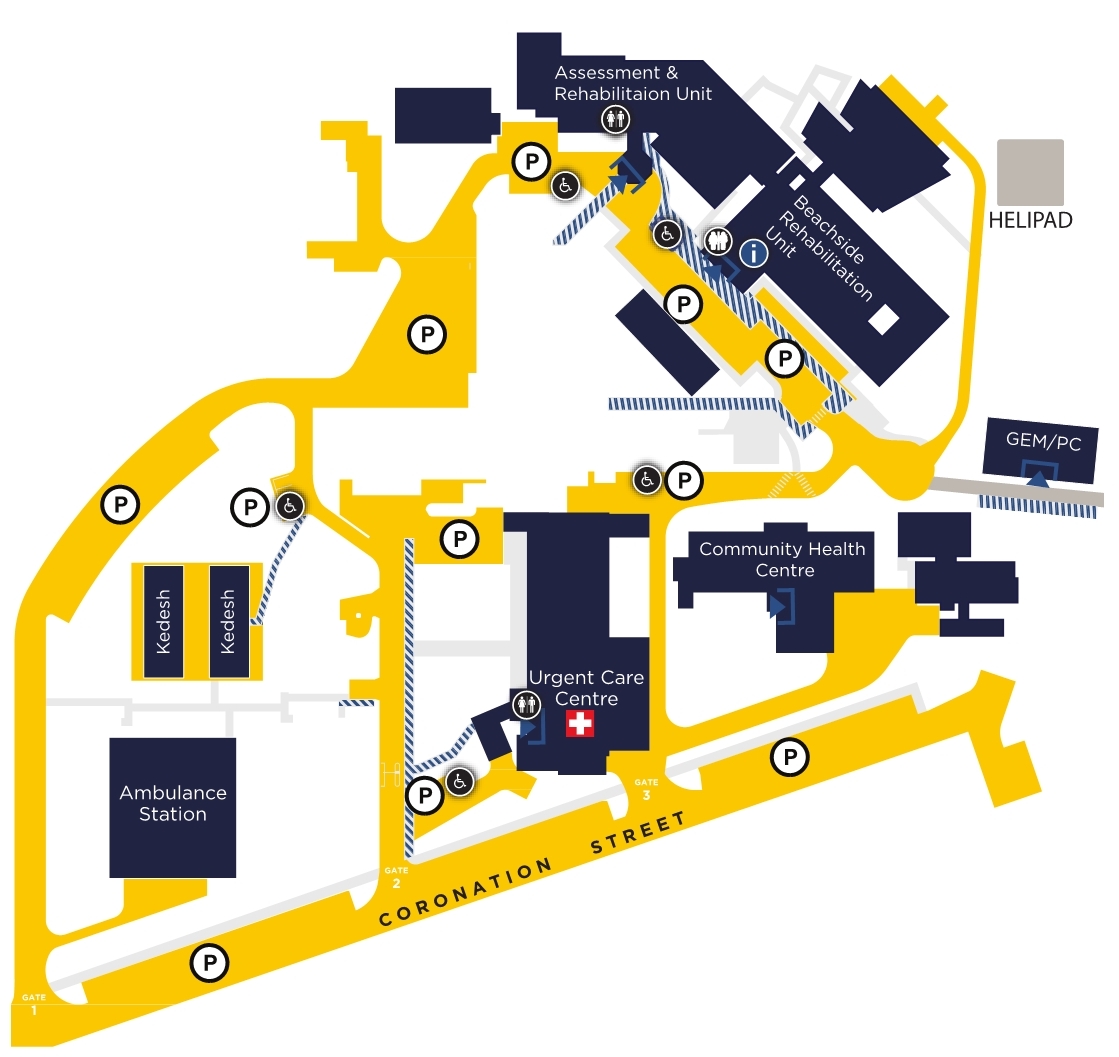
Mona Vale Hospital site map - current. Image: Northern Sydney LHD
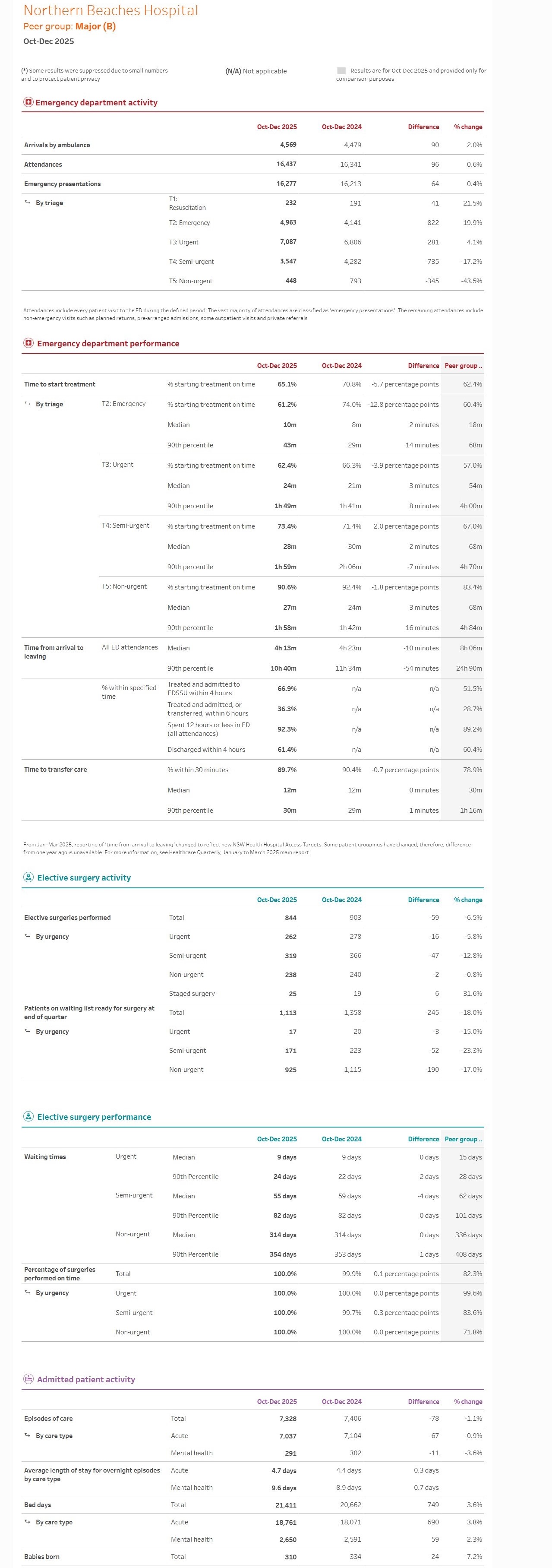
Data for NBH and the NSLHD for the report quarter is:
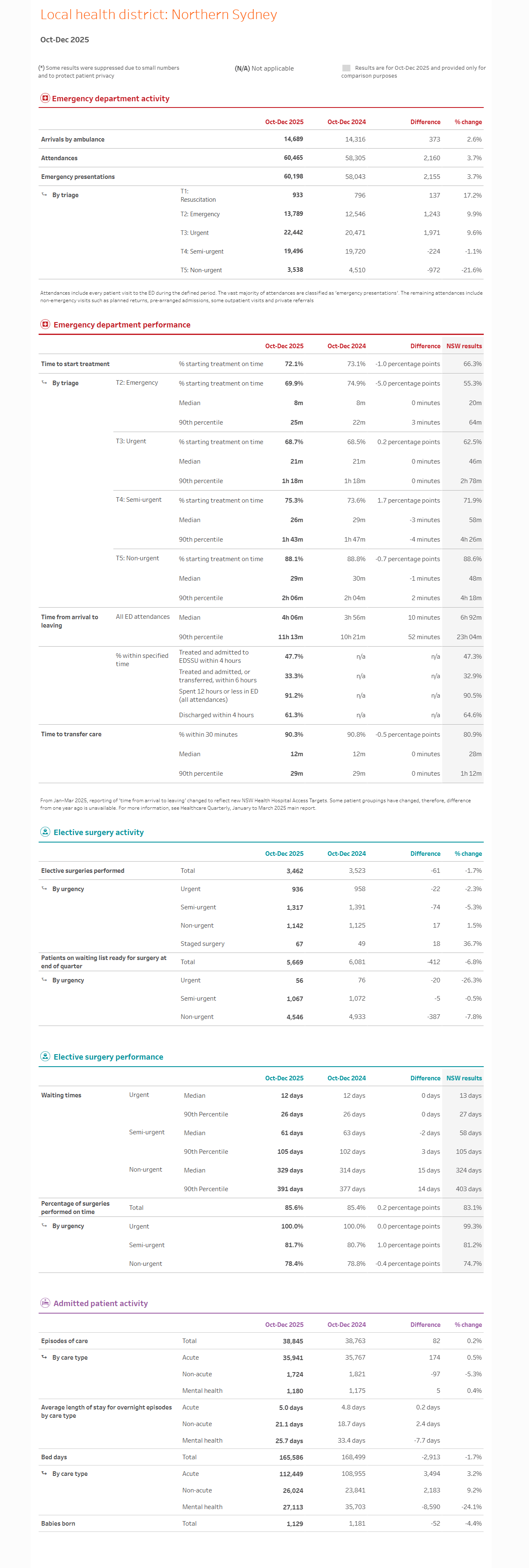
Activity and performance profiles: Northern Sydney Local Health District